Navitus Health Solutions Research: Americans Feel the Pressure of Expensive GLP-1s
GLP-1 medications, including Ozempic, Wegovy, Mounjaro and Zepbound, have reshaped treatment for millions of Americans living with type 2 diabetes and managing weight. Positive clinical outcomes and widespread direct-to-consumer (DTC) advertising have fueled high demand.
But cost is increasingly defining Americans’ experience with GLP-1s.
To better understand how the expense of these revolutionary drugs shapes real-world decisions, we surveyed 2,000 Americans who have used or are using a GLP-1 medication. The findings from our new Pulse Survey show that GLP-1 cost is affecting not only Americans’ wallets but also their access to needed treatment.
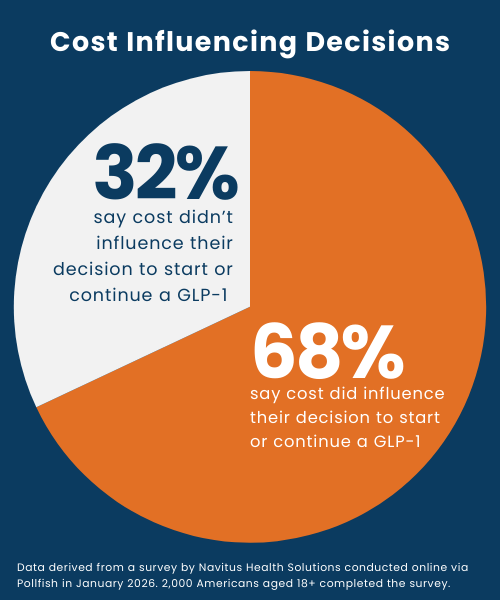
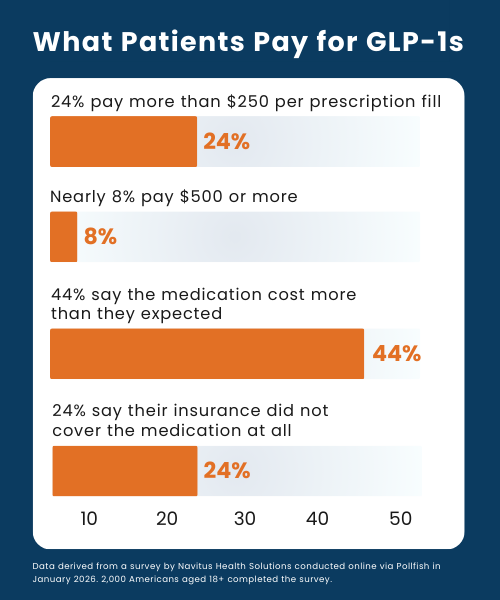
68% of respondents said cost influenced their decision to start or continue treatment. In addition, 24% said they pay more than $250 per prescription fill for their GLP-1, including nearly 8% who pay $500 or more. Those using GLP-1s for weight management were nearly twice as likely to report paying $250 or more per fill compared with those using the medication to manage diabetes.
44% said their GLP-1 medication costs more than they expected, and 24% said their insurance did not cover any of the cost. Among those who stopped taking a GLP-1, cost was the most frequently cited reason, surpassing experiencing side effects or achieving a desired weight. In addition, 60% of respondents said they know someone who wants to take a GLP-1 but cannot afford to do so.
“GLP-1 medications offer meaningful health benefits, but this survey highlights trends related to cost and insurance coverage that introduce uncertainty for a patient’s ability to access these drugs,” said Sharon Faust, Chief Pharmacy Officer at Navitus Health Solutions. “Difficult tradeoffs exist for patients and plan sponsors alike.”
Faust added, “We anticipate demand for GLP-1s will only increase in coming years. This trend will challenge employers, health plans and drug manufacturers to balance access and affordability without compromising clinical support and oversight to patients when medications are covered by insurance.”
The poll findings echo Navitus’ most recent Drug Trend Report, which cited growth of GLP-1s, especially higher-cost, brand-name products, as one of the biggest drivers of overall drug utilization and cost.
With cost becoming a significant barrier, GLP-1 users increasingly are exploring direct-to-consumer programs and other channels for reducing out-of-pocket expenses. The survey found:
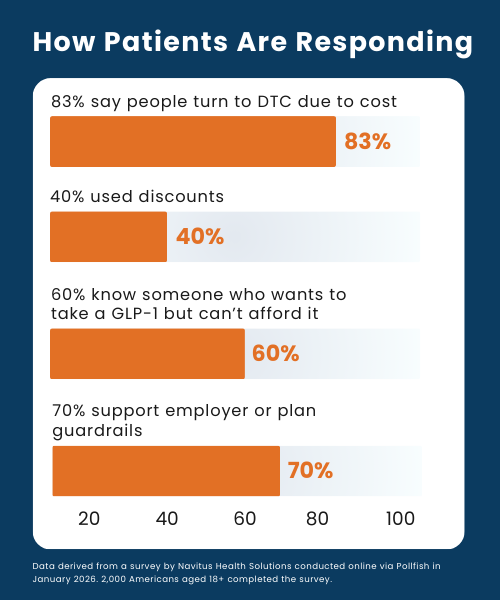
- More than 83% said they think Americans are turning to DTC programs for GLP-1s because traditional health care access is too difficult or too expensive.
- Nearly 40% said they have used discount programs or manufacturer coupons to help offset their out-of-pocket costs.
At the same time, respondents expressed concern about possible risks associated with lower-cost, compounded GLP-1 products often available through alternative programs but not approved by the U.S. Food and Drug Administration (FDA).
Some GLP‑1 medications are compounded outside the FDA process and do not meet the same quality or safety standards as FDA‑approved drugs. Regulators have raised concerns about inconsistent dosing, contamination and storage issues that could put patients at risk. Earlier this month, the FDA announced plans to limit the ingredients used in these compounded products and to step up enforcement against their marketing, noting that the agency cannot verify their quality or effectiveness.
In the Pulse Survey, nearly 60% of respondents said they are aware of potential safety risks of non-FDA-approved GLP-1s, and 86% said they would be willing to pay more for the FDA-approved medications.
Pharmaceutical manufacturers and telehealth providers have also begun offering direct-to-consumer or telehealth-enabled access, bypassing traditional pharmacy benefits and insurance. These new channels can include virtual evaluations and home delivery of medication. While that can reduce administrative friction and lower out-of-pocket costs, these new channels have also raised concerns.
“We have to consider what this means for coordinated care,” Faust said. “Reducing costs and barriers is valuable. But managing complex therapies such as GLP-1s outside traditional benefit and monitoring systems can create gaps in follow-up and oversight.”
The Pulse Survey found that Americans recognize a need for some management of access to GLP-1s. More than 70% said they support employers and insurance programs setting minimum requirements, including prior authorization, thresholds for body mass index or participation in wellness programs, for coverage of GLP-1s.
This finding suggests that Americans understand the sustainability challenges facing employers and health plans as GLP-1 use expands.
“Without thoughtful benefit strategies, affordability challenges will continue to grow,” Faust said. “Employers, health plans and manufacturers must work together to manage costs responsibly while protecting access for patients who need these medications most.”
She added, “This isn’t simply a question of access or restriction. It’s about designing benefits that are clinically appropriate, financially sustainable and transparent for everyone involved.”
About the survey
The Navitus Health Solutions Pulse Survey questioned 2,000 U.S. adults who are taking or have taken GLP-1 medication in the last two years, including for diabetes treatment and weight management. The survey, conducted in January by Pollfish, has an error margin of plus or minus 2.2 percentage points. Error margins are higher for subgroups within the overall sample. Navitus Health Solutions commissions regular Pulse Surveys on health-related topics important to Americans to provide useful data and insights into issues shaping healthcare access, affordability and benefit design.

MORE ABOUT Sharon Faust, PharmD, MBA, CSP
Sharon Faust is the Chief Pharmacy Officer at Navitus Health Solutions. She oversees Health Strategies, Provider Services and Lumicera Health Services. She is a licensed pharmacist in Wisconsin and is on the Board of Directors for the National Association of Specialty Pharmacy and the Drug Selection Advisory Committee for CivicaScript®. In 2023, she was awarded the top 50 most influential leaders in Pharmacy award presented by the Pharmacy Podcast network.
Stay Informed and Connected
Receive expert insights, healthcare tips, and important updates on pharmacy benefits, drug recalls, and more—straight to your inbox.
CLARITY FOR ACTION
Gain Clarity: Navitus 10th Annual Drug Trend Report Ready to Download
Our 2025 report provides transparent, data-driven insight to help plans, plan sponsors and consultants navigate an increasingly complex prescription drug landscape.




